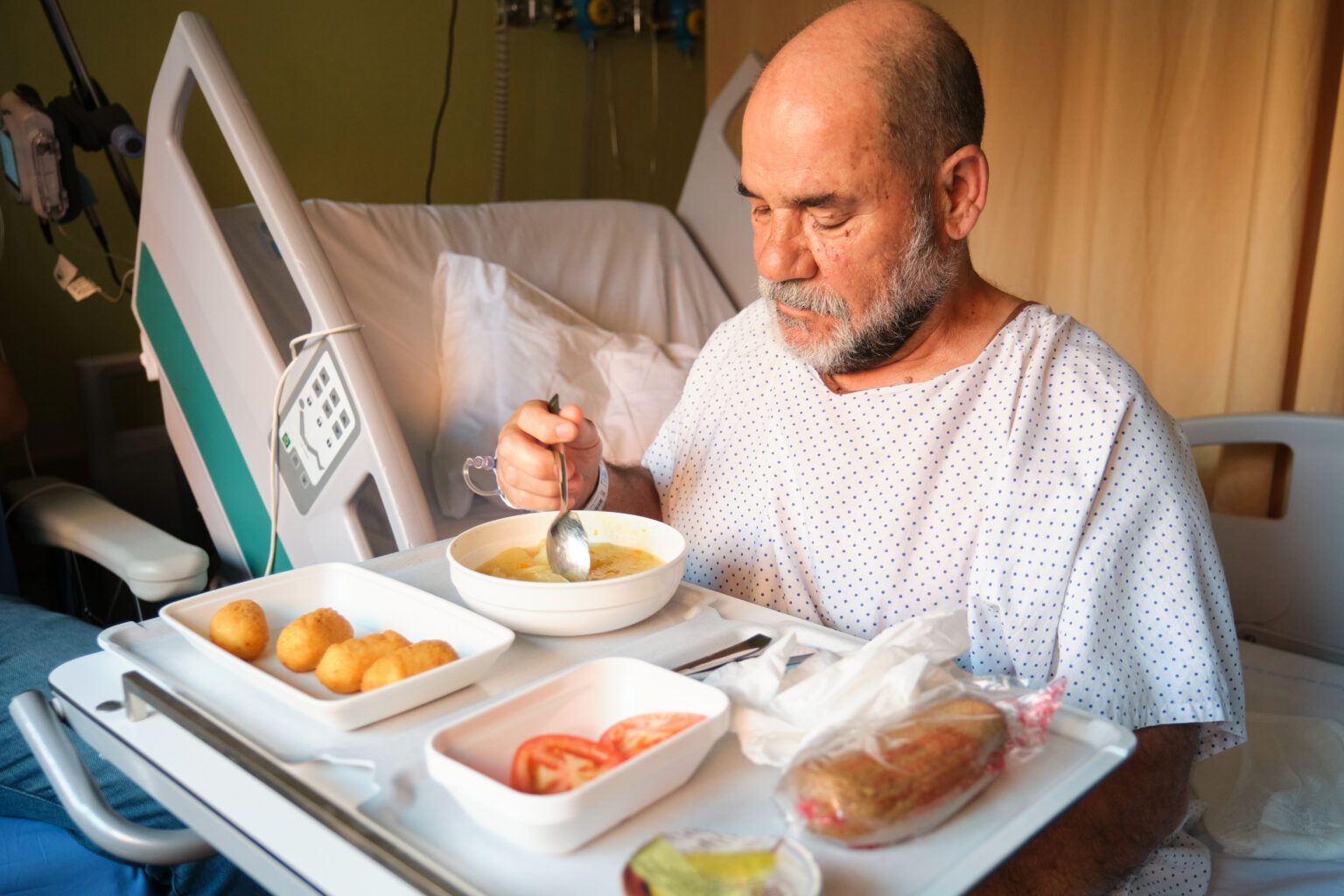
There is no question that a proper diet is an important part of achieving and maintaining good health. But there are limits to that notion.
Last week, the U.S. Department of Health and Human Services (HHS) issued a memo requiring hospitals to improve the quality of food served to patients during hospitalization. This comes as HHS has turned the food pyramid upside-down.
And there are several initiatives within the federal government to reassess the evidence behind many commonly recommended medical practices and ensure that new approvals are based in science.
But here is the problem with this. There is no data showing that a few days of healthy food during a hospital stay makes any difference. Every single reference provided by HHS refers to long-term outcomes from dietary changes, with not one referencing the effect of a short-term diet adjustment.
In fact, a recent literature review found that one common practice, giving patients hospitalized with heart failure a low-salt diet, made absolutely no difference in outcomes. In addition, the data was so compelling that the Society of Hospital Medicine added low-salt diets to their list of “Things We Do For No Reason.”
In addition, as we all know, hospitals are highly scrutinized on their patient experience and satisfaction. So, imagine that you have a patient hospitalized with newly discovered cancer.
And now their meal arrives, and it is, as HHS suggests, “a lentil- or bean-based entrée with leafy greens and olive oil vinaigrette” or “plain yogurt with fresh fruit,” served with unsweetened tea. Have we improved this patient’s outcome or improved their hospital experience? I think not.
Now, should patients receive dietary education during their stay? Absolutely. Should every American have ready access to healthy food, so they don’t have to grocery-shop at the Dollar Store? Absolutely.
But without data, forcing a specific diet on a hospitalized patient is not a sound requirement.
Moving on, I have talked way too much about the Wasteful and Inappropriate Service Reduction (WISeR) program, whereby the Centers for Medicare & Medicaid Services (CMS) has contracted with artificial intelligence (AI) companies to perform prior authorization in six lucky states.
Well, as many may have predicted, the rollout is not going swimmingly. And in fact, one organization, the Electronic Frontier Foundation, has sued CMS to get details on what is happening behind the scenes.
The group states that in Texas, only 62 percent of prior authorization requests are being approved by AI, with half of the denied requests then being approved once a human reviews them. They compare that to Medicare Advantage (MA) plans, which approve 92 percent of prior authorization requests. When you perform worse than MA, that’s saying something.
This group, citing the risks to underserved populations and protected classes, wants to know how the AI algorithms were trained, how the AI companies are being paid, and how the data is being protected.
Finally, the 2027 proposed rules are starting to appear. I skimmed them, and the only interesting thing was in inpatient rehabilitation. The big change is that they are proposing that all therapy modalities must begin within 36 hours of the day of admission, and the first interdisciplinary team meeting must be within four days of admission.
I am sure that there are other noteworthy items, but there are only so many hours in a day.
EDITOR’S NOTE:
The opinions expressed in this article are solely those of the author and do not necessarily represent the views or opinions of MedLearn Media. We provide a platform for diverse perspectives, but the content and opinions expressed herein are the author’s own. MedLearn Media does not endorse or guarantee the accuracy of the information presented. Readers are encouraged to critically evaluate the content and conduct their own research. Any actions taken based on this article are at the reader’s own discretion.